Karen Barrie, Health and Social Care Alliance Scotland
Working with the National Patient Experience Programme, I was often asked to support service improvement projects. One improvement initiative called LEAN took place in an inpatient rehabilitation unit for people with acquired brain injury. An earlier patient experience survey had generated extremely positive results, making it difficult to identify areas for improvement. A subsequent focus group also produced positive findings. While staff were grateful to receive such positive feedback, they felt that there was still room for improvement. So I was asked to do more research in the hope that probing aspects of patient experience in detail might uncover specific improvement actions. Checking through the results of the earlier focus group, it was clear that all environmental and relational aspects of care had already been probed in depth. So we agreed to switch to a different lens, from what the service did to what people were enabled to feel and do.
I carried out eight interviews with a deliberately diverse mix of people who had recently passed through the service. The interviews were open, but I ensured that the three types of outcomes in the Talking Points framework were covered by asking follow-up questions. The interviews were recorded and then typed up and when I started analysis of the interviews, I read through the data as follows:
- Looking for emphases, elaborations and repetitions within accounts
- Looking for repetitions and similarities across accounts
- Looking for differences between accounts
- Clustering related issues
- Using the Talking Points personal outcomes framework as an organising guide/identifying what was missing from the accounts.
The eight accounts confirmed and expanded on the earlier findings: without exception, staff were regarded as exemplary. There was a committed rehabilitation ethos across staff groups, including domestic staff, with nursing staff keen to support exercise practice back on the ward. Consequent change outcomes centred on improved mobility and function (especially cognitive functioning) and increased confidence. Morale improved as a result of a sense of achievement, the gradual return of hope, and process outcomes, including feeling valued, motivated and encouraged. Anticipated process outcomes such as feeling listened to or having a say however featured less prominently, because many people identified that they were happy to take a lead from staff in terms of therapy.
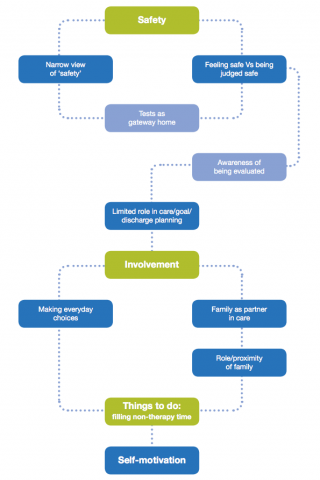
From an improvement perspective, three main inter-related themes emerged: safety, involvement and having things to do during non-therapy time, as illustrated in the diagram below.
When findings were fed back to staff, they recognised that there was a tendency within the service to focus narrowly on physical safety; the priority was ensuring that people were safe to function at home, as often there was a pressure on beds. It was reported in the interviews that people felt pressurised by the test in hospital to check whether they were able to function in the kitchen. Until this point, the therapy staff had not been aware of the emphasis elsewhere in the service on 'passing the kitchen test' or the fact that it was causing anxiety. They were able to identify the source of this issue and undertook immediate steps to address it.
Another issue that was highlighted several times was the tension between being judged safe by staff within the hospital, and the subjective outcome of feeling safe. For example 'I was told 'you're safe to go home now'. But I didn't feel safe at all. An elderly neighbour who lived directly below was unwell at the time, and I was really worried what might happen to him if I had a relapse'. This mismatch between perspectives resonated strongly with staff, who reflected on the lack of transparency regarding how patients are assessed for their readiness to return home while in the hospital, and how communications might be improved.
Two of the identified themes also presented an opportunity to inform previously identified LEAN actions. The LEAN work had highlighted 'poor use of non-therapy time', resulting in a suggested action to involve families in weekend exercise practice and perhaps introduce a programme of activities. The interview analysis however suggested that while the introduction of further planned activities would perhaps relieve boredom and accelerate functional improvements, it would further compound the limited opportunities for people to exercise choice. It was, therefore, agreed that a focus group involving former patients, relatives and staff would explore these themes further.
The focus group confirmed that a planned programme of activities would not be helpful as fatigue levels were problematic and unpredictable. There was also a strong feeling that nursing staff were already very supportive of exercise practice. While some people had used family visits and outings to practice everyday life skills, from ordering and paying for coffees, to treating a trip to the hairdressers as a 'social test', this was not universal. As one relative remarked 'See, we just thought it was good for her to have a change of scene. I mean, we would never have thought of doing anything like that, but I can see how it would have helped'. Because encouragement and support to do this was considered valuable, it was agreed it should be more widespread. While former patients recognised that, due to their brain injuries, they had often lacked sufficient awareness to engage in formal goal setting, several ways of allowing opportunities to make simple choices were jointly identified by staff, former patients and relatives. Interestingly, it was also agreed that staff preparation of individualised colour-coded weekly timetables should be phased out in the run up to discharge. Although former patients had viewed them positively, it was recognised that the change from fully programmed to completely unstructured days was too abrupt, and also did not support making and keeping appointments in the outside world.
This short piece of analysis highlighted the importance of focusing on outcomes, as well as experience of, and attending to, what was not said. The Talking Points Framework was invaluable in supporting this.